Creating a safe sleep environment is one of the most important precautions you can take for your baby. These safe sleep guidelines for babies can help you to reduce the risk of sleep-related accidents. Here is what you need to know!
As a new parent, you want your baby to be healthy and out of harm’s way. We babyproof our homes to keep our little explorers protected from possible dangers, and we look for the safest car seat. Similarly, we need to take deliberate steps to create safe sleeping environments. A big part of making sure your baby is safe occurs when they’re asleep. It’s important to follow the safe sleep practices laid out by the American Academy of Pediatrics (AAP) and other organizations compiled here to decrease the risk of sudden unexpected infant death (SUID) and sudden infant death syndrome (SIDS).
This article has been reviewed by Dr. Gina Jansheski, M.D., FAAP
Explaining SUID and SIDS
I know that these are the two most anxiety-inducing topics of early parenthood. But, like all baby health and safety topics, it’s good to be aware and proactive when it comes to safe baby sleep.
So let’s get into the medical stuff first. SUID is an umbrella term attributed to death by suffocation, asphyxia, entrapment, infection, toxic ingestions, metabolic diseases, cardiac arrhythmias, and trauma (unintentional or nonaccidental). SIDS is a subcategory within SUID, which is when the cause of death is unknown or unclear. It’s important to be aware that these terms pertain to those babies 1-year-old and younger. For simplicity, we will use the term SIDS throughout this article to encompass both SIDS and SUID.
While these make up the number one cause of death in infants younger than one year of age, they are still rare. I always had to remind myself of this when I had a young baby in the house. These tragedies do happen, but not as often as we parents would fear; approximately 3,600 babies die unexpectedly each year in sleep-related incidents in the United States. The key is that a number of these deaths could have been prevented.
With this in mind, you can decrease your baby’s risks by following safe sleep guidelines. Personally, I have always felt empowered by this—every parent and caregiver can take an active role in keeping babies safe as they sleep.
(A note to readers from outside the United States: Please refer to the guidelines set by your country’s national pediatric association.)
Safe Sleep Isn’t Just About Your Baby’s Sleep Environment
Before we go over the safe sleep guidelines for babies, let’s review some of the other important factors that go into ensuring safe sleep for babies.
“Safe infant sleep ultimately begins with a healthy gestation.”
—Dr. James McKenna
There are many things during pregnancy and after birth that may seem completely unrelated to sleep but will play a big role in your baby’s overall health and safety, including SIDS risk. Here are some important steps you can take to ensure that your baby is set up for safe sleep success.
Get regular prenatal care during your pregnancy.
By seeing your doctor for regular prenatal care, you will have a better chance for a healthy pregnancy and baby. Nutritional deficits, low-birth weight, and prematurity are all linked to SIDS.
Avoid cigarette smoke, alcohol, and illegal drugs.
Smoke exposure is a major risk factor for SIDS, especially maternal smoking. Fetal exposure to cigarette smoke increases the risk of preterm birth and low birth weight, both of which are significant risk factors for SIDS. In fact, it is estimated that one-third of all SIDS deaths could be prevented if maternal smoking was eliminated.
It is estimated that one-third of all SIDS deaths could be prevented if maternal smoking was eliminated.
Simply put: you must avoid smoking and smoke exposure during pregnancy and once your baby is born. Don’t smoke, and set firm boundaries with loved ones who might smoke or be around smoke. Keep your entire home, work environment, and car smoke-free. Don’t go where you’d be exposed to cigarette smoke, such as a bar or casino.
As you might guess, using alcohol and drugs will also increase the risk of SIDS. Several studies have examined these factors, and the answer is always an increased risk. One such study demonstrated that babies born to mothers who smoked and drank beyond the first trimester have a 12-fold increased risk for SIDS. And when a baby bedshares with a parent who drinks alcohol, uses sedatives, or takes illicit drugs, they are at particularly high risk.
Additionally, maternal alcohol use during pregnancy is the number one preventable cause of intellectual disabilities in children. I know that there are statistics that would lead someone to believe that alcohol intake during pregnancy may not be dangerous, but the fact is that no amount of alcohol use is safe during pregnancy. Since a baby’s organs are still developing during pregnancy, your baby’s liver isn’t capable of handling alcohol of any kind (including wine, vodka, tequila, and other spirits). In fact, it’s easy to assume that fetal alcohol syndrome (a severe condition resulting from exposure to alcohol in the womb) is rare, but it affects 1 in 100 babies in the United States, making it significantly more prevalent than SIDS.
Practice skin-to-skin care with your baby.
Skin-to-skin care, also called kangaroo care, is the practice of laying your baby belly-down on your bare chest for prolonged, direct skin contact. The AAP recommends practicing skin-to-skin with your baby after birth, regardless of whether you had a vaginal or c-section delivery. Your partner can fill in and practice skin-to-skin contact after your baby’s birth if you are unable to do so for any reason.
This is usually done immediately after birth, during what is known as the “golden hour,” but there are tremendous benefits to continuing this practice during the early weeks at home with your baby. Skin-to-skin care has been linked to lower mortality rates, easier breastfeeding, better thermal regulation, mental boosts, and healthier weights. For example, preemies who had received skin-to-skin care were found to have better brain functioning at adolescence than controls who did not receive this special intervention.
Practicing skin-to-skin care with your baby as often as possible during the first few months of life can be an important part of your baby’s health for years to come, including reducing your baby’s SIDS risk in the first year.
Do everything possible to breastfeed your baby.
Let’s also emphasize how important breastfeeding is in the overall health and well-being of your baby—and yes, this even applies to safe sleep.
A large review study concluded that breastfeeding for at least 2 months leads to a reduced risk of SIDS by up to 50%! And the longer you breastfeed, the more protective effect is seen. So, you should breastfeed exclusively or feed with expressed breastmilk for at least 6 months if possible and feasible. The same study points out that even partial breastfeeding (breastmilk and formula feeding) can reduce a baby’s risk of SIDS. In fact, more than 900 infants per year may be saved in the US if 90% of mothers exclusively breastfed for 6 months.
I acknowledge that breastfeeding isn’t always easy and whether you breastfeed your baby is your decision, but if you can breastfeed or pump your breast milk, it certainly will help your baby in a number of ways, including promoting safer sleep. If you are struggling to breastfeed, please check out our breastfeeding section for articles like breastfeeding tips for new moms and how to boost your milk supply.
Practice regular tummy time with your baby.
Pediatricians recommend daily supervised awake tummy time, and this is an important way to help your baby sleep more safely. Get your little one on the play mat or play gym and have fun! Tummy time helps build shoulder and neck strength. As you might guess, the stronger these muscles are, the better your baby can navigate their sleep environment.
12 Important Safe Sleep Guidelines for Babies
The American Academy of Pediatrics has provided research-backed guidelines for safe infant sleep, and I’ve included some other resources to help you as well. I encourage you to follow these practices to substantially decrease your baby’s risk of sleep-related death or injury.
1) Always put your baby to sleep on their back.
Thanks to the Back to Sleep Campaign, an initiative that was launched in 1994 to encourage putting babies to sleep on their backs, the incidence of SIDS has declined by more than 50%. That’s an amazing statistic for such a simple intervention, and it really gives parents a lot of power to decrease their baby’s risk of SIDS. I think it’s remarkable that a simple act can have such a big impact on sleep safety!
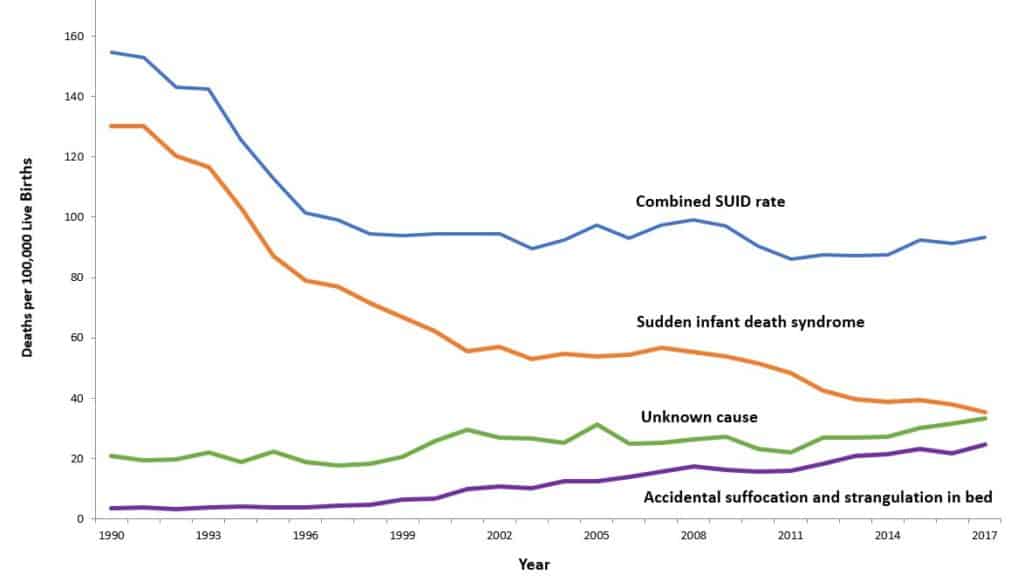
As you can see, there was a significant decrease in the combined SUID rate and SIDS rate beginning in 1994 when the Back to Sleep campaign first launched.
So you should always place your baby to sleep in a supine position (on the back) for every sleep, and make sure that every caregiver does the same (do talk about this with grandparents and other family caregivers, as well). This sleep position does not increase the risk of choking in infants. Even babies with gastroesophageal reflux do not have issues with this position because of the natural airway mechanisms that protect against aspiration.
The AAP also explains that prone sleeping (stomach-sleeping) and side-sleeping are not safe. Contrary to what people used to think, stomach-sleeping can contribute to difficulty breathing and lead to decreased airflow and even suffocation. Similarly, if your baby sleeps on his side, he can accidentally roll over onto his stomach without knowing how to turn his head to breathe.
It’s recommended that you continue to place your baby on his back for sleep, even if he rolls over to his stomach on his own. Most doctors will tell you that once your baby can roll over to his back independently, you don’t need to reposition him in his sleep if he rolls onto his tummy, but you should immediately stop using a swaddle. Babies typically start rolling over between four and six months old, but they begin moving around when they wake up even earlier, and you never know exactly when it will happen. This is a good reason to keep your baby’s sleep space clear and free of toys, blankets, pillows, and bumpers from day one.
2) Use a firm, clean, CPSC-approved sleep surface.
An approved sleeping surface for an infant is a crib, bassinet/Moses basket, or portable crib. Follow the manufacturer’s guidelines when using these sleep products, and revisit them when your baby gains new skills. For example, you’ll need to stop using a bassinet once your baby starts pulling up, and you should use a lower crib mattress height at that time, too.
In the United States, it is the Consumer Product Safety Commission (CPSC) that decides a sleep surface is safe for babies after the product passes federal standards. If it fails to pass the appropriate standards, the product would not be approved for infant sleep. Products labeled sleeper, napper, nest, co-sleeper, etc., have not passed these standards and are not approved for safe sleep.
What qualifies as a firm sleep surface?
Place your baby on a firm sleep surface (such as the CPSC-approved ones listed above) covered by a fitted sheet and nothing else. A firm surface means that it maintains its shape and will not indent or conform to the shape of the baby’s head. If your baby’s sleep surface creates an indentation, it will increase the risk of rebreathing air, which is one of the proposed mechanisms for SIDS.
Very important to note is that you should always use the mattress designed for the specific product. For example, you may find aftermarket bassinet mattresses, but they have likely not been tested for safety with the bassinet you bought. The bassinet manufacturer should have the most reliable information on this, so you could contact them and ask which mattresses are approved for use with their product.
Make sure the mattress passes the gap test
Another important safety check is to make sure that there are no gaps between the mattress and the wall of the crib, bassinet, portable crib, or play yard. For a crib, you shouldn’t be able to fit more than two fingers between the crib and the mattress. Any bigger than that means the mattress is too small for the crib.
Federal safety regulations to know about
Each type of safe sleeping surface for infants has its own set of federal safety regulations and guidelines. And there is a long list of safety measures and requirements that must be met. I won’t list them here, but I think it’s useful to take a look at the safety standards for a baby sleep product. You can see for yourself the detailed requirements that manufacturers must meet to make a sleep surface as safe as possible for your baby to sleep in.
The federal safety regulations for full-size baby cribs can be found under 16 CFR Part 1219, while the safety regulations for a non-full-size baby crib fall under 16 CFR Part 1220. Play-yards are subject to 16 CFR Part 1221.
3) Have your baby sleep in your bedroom for the first 6–12 months.
The AAP recommends that your baby should sleep in your bedroom for the first year of life or at least the first six months. This allows you to watch your baby and comfort her. It also makes middle-of-the-night feeding sessions much easier. By sleeping in the same room as your baby, the AAP says you can decrease the risk of SIDS by as much as 50%.
Personally, I felt much better hearing my baby next to me, making all those cute dinosaur grunting noises as he slept. At first it kept me awake, but I soon became adjusted to it and found it reassuring over time. And when it was time to breastfeed, it was so much easier because I usually sat up, made some space in my bed, nursed him, and then put him back in his bassinet.
Now, I recognize that it can be difficult to stay awake during those middle-of-the-night feedings. I have definitely fallen asleep with my baby in bed, and even the AAP recognizes that this will happen and recommends that you put your baby back in the bassinet as soon as you wake up. But you should try your best to avoid this.
That’s why, as a precaution, it’s prudent to remove any and all safety hazards from your bed if you might be bringing your baby into it with you for a nighttime feeding. This includes removing all loose bedding and pillows and ensuring there are no wires or loose items in the bed or large gaps around the mattress.
To avoid falling asleep while nursing your baby, it helps to sit up with a nursing pillow or even turn on dim lighting (amber or red lights are the best for nighttime use) while you feed your baby at night.
Struggling with your baby’s sleep? I’m here to help. Join my affordable holistic sleep membership, the Gentle Sleep Society, for expert guidance, practical tips, and a supportive community. Use code GENTLESLEEP to save $10 today and start your journey to better sleep!
4) Avoid sedatives, alcohol, illicit drugs, smoking, and smoke exposure.
It’s easy to downplay a glass of wine, a melatonin pill, a joint, a cigarette, or even a sleeping pill. It’s “just one glass” or “just one cigarette.” Or it’s “I really need this to sleep.” But these substances are dangerous if there is a baby in your home, and they can increase SIDS risk.
Mama, it is imperative that you and your partner and all caregivers avoid these substances at all times. In addition to sobriety being the primary caregiver’s responsibility, other adults in the home must also hold themselves to these same standards or maintain a careful distance from the baby to prevent exposure or dangerous incidents.
Avoid cigarettes, marijuana, and vaping
Do you or your partner smoke cigarettes, e-cigarettes, or marijuana? A German study from 1990 found that almost 29% of women smoked throughout pregnancy. And a more recent examination found that this figure has decreased to 10% since 2010. These statistics were shocking to me.
If you (or your partner or any other adult in your home) smoke cigarettes, marijuana, e-cigarettes, or anything else, you need to quit now that you’re pregnant or you have a baby in the home. Even if you or your partner only smoke outside and away from the baby, for example, your baby will still be exposed to the chemicals in secondhand smoke.
Cigarette smoke contains about 4,000 chemicals, including nicotine and carbon monoxide, and it should be no surprise that smoke exposure not only puts your baby at risk for birth defects, low birth weight, and pregnancy complications, but it is a major risk factor for SIDS. Exposure to cigarette smoke, whether during pregnancy or secondhand smoke after birth, interferes with an infant brain’s ability to regulate their breathing and affects their ability to wake up from sleep. Terrifying! That cigarette just isn’t worth the damage it will do to your baby.
In fact, the CDC states that “Infants who die from SIDS have higher concentrations of nicotine in their lungs and higher levels of cotinine (a biological marker for secondhand smoke exposure) than infants who die from other causes.”
E-cigarettes contain nicotine, propylene glycol, formaldehyde, and other chemicals, but no studies to date have been conducted that look at their impact on SIDS risk. But, that doesn’t mean that smoking these won’t have the same or similar effects on a baby’s brain, lungs, and sleep arousal as cigarettes do.
Marijuana contains about 400 chemicals, and there is a significant association with SIDS if dad smokes during conception, pregnancy, or after birth. According to the American College of Obstetrics and Gynecology (ACOG), when mom smokes or consumes marijuana during pregnancy, the chemicals cross the placenta, and there is a higher chance for a stillbirth or preterm birth or for her baby to be born with lower birth weight. ACOG is against the use of marijuana use during prepregnancy, pregnancy, and lactation periods.
As for whether a mother’s marijuana use contributes to SIDS, it may be a risk factor, but more research is needed. However, that is not a green light to use marijuana because it is known that marijuana use disrupts brain and nervous system development and there is no safe level of marijuana during pregnancy or lactation.
And when a breastfeeding mother uses marijuana, THC transfers through breast milk and is metabolized by the baby, so this exposure can have long-term consequences on their health. Additionally, secondhand marijuana exposure may have the same effects on children as secondhand cigarette smoke (according to ACOG). For all of these reasons, mothers and fathers should not smoke or consume marijuana during pregnancy or after birth.
The bottom line: I can’t emphasize enough how important it is that you do not smoke or expose your baby to someone who smokes, including your partner or another family member or friend.
The effects of smoke exposure are harmful enough, but if you bedshare, this dramatically increases your baby’s risk of SIDS. A baby who bedshares with an adult who smokes (even if that person does not smoke in bed) has a very high SIDS risk. Take, for example, this statement on bedsharing with parents who smoke from an analysis of five studies on bedsharing:
“Infants who bed share at 2 weeks of age and whose parents both smoke are at 65-fold increased risk of SIDS compared with infants room sharing with parents who do not smoke.”
Having a baby and smoking cigarettes, marijuana, e-cigarettes, or other substances don’t mix. Protect your baby by avoiding these altogether.
Avoid drugs and alcohol
Take caution with anything brain-altering. If you or your partner drinks alcohol, that can increase your baby’s SIDS risk, and the same goes for illicit drugs, certain prescriptions, and over-the-counter medications. For example, if the label says you shouldn’t drive when you take this medicine, you shouldn’t care for a baby while using it, either. Talk to your doctor about safer alternatives.
Maternal first-trimester binge drinking was also found to be associated with an increased SIDS risk. A study from Denmark has shown a significant relationship between infant mortality and maternal binge drinking. Maternal alcohol use has been shown to increase the risk of SIDS deaths and even non-SIDS infant deaths. And just like with cigarettes, parents who consume alcohol or illicit drugs and bedshare place their baby in a much higher SIDS risk category.
Even sedatives, pain medication, and other drugs can be risky because they can inhibit or alter your brain activity; additionally, supplements like melatonin may also cause you to be less alert or to be in a deeper state of sleep. You may not realize it, but these may impair your judgment or alertness, and you may not be able to care for your baby safely while using these substances.
I know that melatonin, for example, is a common natural sleep aid. But every time I’ve taken it, I’ve been in a really deep sleep state and groggy for hours after waking. Even though my kids aren’t babies anymore, I feel that it would be irresponsible for me to take this as their mom because of the way it affects my body and my brain.
Set firm boundaries to protect your baby
All of these exposures are preventable. If you are having trouble setting boundaries with family or friends, or even your partner, please read The Newborn Nine: 9 Important Rules for Visiting a Baby. If someone doesn’t respect one of your boundaries and violates one of these rules, you could simply say, “Nope, sorry. That’s one of the newborn nine rules that places my baby in danger, and I can’t allow that.”
You could even share this safe-sleep guidelines article or the rules article with them because that’s what I wrote these for! It’s hard enough to be a new parent… on top of everything you already have on your plate, you shouldn’t have to deal with people not respecting your wishes or your boundaries. As unpleasant as it can sometimes be, setting boundaries and advocating for your child is something you might as well learn now, as it will affect you throughout your baby’s childhood with babysitters, at school, with friends and their parents, and beyond into the teenage years.
5) Don’t share a bed with your baby.
Even in the absence of hazards in or around the bed, the AAP is opposed to bedsharing. This is because bedsharing is associated with factors such as loose/soft bedding, head covering, and increased exposure to smoke if the parents smoke, leading to an evidence-based increase in the risk of sleep-related death. Bedsharing also increases the risks for unintentional injury and death, such as suffocation, asphyxia, entrapment, falls, and strangulation, especially for babies under 20 weeks of age.
Want to Save This Post?
In fact, an analysis of five case-controlled studies that examined the safety of bedsharing without hazards states: “Bed sharing for sleep when the parents do not smoke or take alcohol or drugs increases the risk of SIDS. Risks associated with bed sharing are greatly increased when combined with parental smoking, maternal alcohol consumption and/or drug use. A substantial reduction of SIDS rates could be achieved if parents avoided bed sharing.”
While researchers have suggested that bedsharing promotes breastfeeding in some contexts and may be less risky for older infants if there are no risk factors or hazards in the bed, and even though there are well-known proponents of safer bedsharing such as Dr. James McKenna, the data just doesn’t support bedsharing as a safe sleep practice.
Instead, the AAP encourages room-sharing for the first 6–12 months of your baby’s life, where your baby sleeps on a separate sleep surface in your bedroom, because this can reduce the SIDS risk by as much as 50%. Room-sharing is safer than bed-sharing and safer than having your infant sleep alone in their own bedroom.
I know that many parents end up bedsharing, even unintentionally. A 2010 study found that approximately 60% of mothers bedshare throughout the first year. This is a whopping statistic. What’s more, the La Leche League estimates that many of these instances are unplanned, meaning that the parents did not plan or intend to share a bed with their baby.
If you find yourself in this situation or if you decide to ignore these warnings and bedshare anyway, please refer to the safer bedsharing guidelines from La Leche League and the Mother-Baby Sleep Laboratory for information on how to reduce the risks of SIDS while doing so, avoid smoking and intoxicating substances, and follow the rest of the guidelines in this article religiously.
Personally, I was one of the moms who unintentionally ended up bedsharing after both of my kids were about 5 months of age. There were many safety precautions I didn’t know about and wished I had. Those articles on safer bedsharing will be helpful to reduce some risk factors if you find yourself in a similar position.
6) Keep your baby’s sleep surface free from all objects and loose bedding.
Your baby’s crib or sleep area should be bare-bones. There shouldn’t be any pillows, soft toys, quilts, comforters, loose bedding, or any other loose items in their sleep area. In fact, bedding in the area increases SUID risk fivefold.
For the sleeping area to be safe, it should be very simple: a tight-fitted sheet over an infant crib mattress (or bassinet pad) and a pacifier if your baby uses one. That’s it!
To reduce the risk of SIDS, as well as suffocation and entrapment, do not place any objects in the crib or bassinet. And never use crib bumpers or sleep loungers! A baby can scoot, roll, or turn their head for those extra items to immediately go from cute decor to dangerous hazards.
I know that many new parents may think that it’s safe to have some of those items near the crib when their baby is not yet rolling over. A sweet baby blanket draped over the crib rail or a special stuffed animal sitting in the corner seems comforting and makes a beautiful decoration. After all, a newborn (especially when swaddled) doesn’t really move around the crib. And that might be the case for a day, a week, or longer, but there will be that first time when your little one starts to scoot when you are asleep or not in the room. You won’t be able to predict when that will happen, and you won’t have the chance to remove those objects before they become dangerous.
So, the recommendation is to just keep all items, except for a tight-fitting sheet, out of the crib. Period.
7) Avoid overheating and head covering your baby.
Be sure to keep your baby’s sleep area cool and comfortable. Experts generally advise keeping the temperature in your baby’s room no higher than 72°F, with 65–72°F being the optimal range. You’ll also want to dress your baby appropriately for the environment, with up to one more layer than an adult would need to sleep.
I always suggest good-quality cotton pajamas and sleep sacks. Cotton gives warmth while also providing optimal breathability. The other fabric you can consider for the sleep sack is merino wool. Wool will wick moisture to create a comfortable sleep.
Babies don’t have the same temperature-regulating abilities as older children and adults, so they don’t always sweat when they are hot. I suggest monitoring your baby for signs of overheating whenever you wake up to comfort or nurse your baby.
The best way to see if your baby is too hot is to simply feel the back of the neck and the front of your baby’s chest. If it’s hot to the touch, your baby is likely too warm, and it might be a good idea to lose a layer of clothing or switch to a lighter sleep sack. The neck should feel comfortable and lukewarm to indicate a good temperature for sleep.
Don’t over-bundle your baby, even when it’s snowing outside, and do not cover their face or head. (No hat-wearing to sleep!) The reasoning behind finding the right temperature for your baby is that overheating is linked to SIDS. Research suggests that babies sleep more deeply when they are very warm and can be difficult to rouse to wakefulness. A study of variable risk factors for SIDS found that heating a bedroom increases SIDS risk compared to not heating a bedroom. So always be careful not to over-bundle your baby or let them sleep in a hot environment (this also applies to when they are in the car seat or stroller).
8) Never sleep with your baby on a couch or armchair.
Research has shown that about 1 in 8 sleep-related infant deaths occur on a sofa. The findings suggest that these incidents are usually accidental (e.g., someone fell asleep with the baby on the couch), and those were not planned sleep locations.
If you feed your baby in the middle of the night, you may find it convenient to use the glider in your nursery, but you have to make sure that you don’t fall asleep in there. A safer alternative may be to sit up in bed with your baby or bring your baby into bed with you for a feeding session, provided that you have checked your bed for safety hazards (including loose items, wires, partners who have been drinking, and large gaps between the bed and wall or headboard).
9) Stop swaddling as soon as your baby shows signs of rolling over.
Swaddling your baby to sleep is very calming and encourages them to sleep on their back. But it is not an effective strategy to reduce the risk of SIDS. In fact, you should stop swaddling your little one around 6–8 weeks old. When your baby first shows signs of attempting to roll over, you can continue to swaddle with arms out. This allows your baby to use his arms to help find a comfortable and safe sleep position if and when he rolls over.
10) Offer your baby a pacifier at nap time and bedtime.
Some studies have identified that pacifiers can offer some protection against SIDS. Once breastfeeding has been well-established (usually by about six weeks old), it’s not a bad idea to offer your baby a pacifier at bedtime.
But there is no need to stress if your baby won’t take one. If your baby likes the pacifier, he’ll take it, and if not, he won’t. And that’s OK! It’s just another one of those “it can’t hurt” preventative tactics to try. Note that if the pacifier falls out of his mouth once he’s asleep, you don’t need to reinsert it.
Keep in mind that choosing and trying out different pacifiers might be part of this journey. They come in various shapes, materials, and sizes. You can read my pacifier recommendations to help find the best one for your baby. The safest type is made as one piece. Pacifiers made with two or more components pose some risk of falling apart and becoming a choking hazard.
Additionally, make sure that as your baby gets older, you size up the pacifier to the appropriate age. For example, if your baby is 6 months old, you should not be using a pacifier that is designed for birth to 3-month-olds, because it will be softer and easier to bend, and that can also pose a choking hazard. Equally, you don’t want to use any pacifier clips or attachment pieces (including stuffed animals) for sleep.
11) Circulate the air in your baby’s room.
Some researchers have suggested that room ventilation may be another factor in sleep-related deaths, but the studies have been small (yet promising). The use of a ceiling fan can potentially decrease SIDS risk by 72%.
What does this mean for you as a parent? Though it may not yet be a proven way to reduce your baby’s SIDS risk, and the exact reasons haven’t yet been identified, it would be prudent to circulate the air in your baby’s room during naps and at nighttime.
Here are some ways you can improve the ventilation in your baby’s room:
- Keep the bedroom door open. Keep the bedroom door open in your baby’s room while they sleep to ventilate the room.
- Use a fan. Use a ceiling fan or other fan in your baby’s room, but please note that there isn’t enough data to provide specific recommendations about how, when, or where to place the fan to reduce the risk of infant death (or other risks related to the fan itself). A ceiling fan or small fan with the cord tucked behind a dresser is probably safer than a large, top-heavy floor fan that can tip over or be pulled on when your baby is playing—as long as the fan you choose circulates the air near your baby’s sleep zone. (Of course, keep all cords away from your baby, especially while they are sleeping.)
- Purify the air. In general, keep the air clean in your home. Indoor air quality is up to 5–10 times more polluted than the air outside, so open the windows in your home often and run a HEPA air purifier in your baby’s room.
By keeping the air moving throughout the room, your baby will be less likely to breathe stagnant air or rebreathe exhaled air, factors that may play a role in SIDS risk. Air circulation will also keep your baby cool, which reduces the risk of your baby overheating. Win-win.
12) Do not use home cardiorespiratory monitors as a way to reduce the risk of SIDS.
While popular and now more available, cardiorespiratory monitors have not been shown to reduce SIDS. These include the Snuza, Owlet, and the Angel monitors. The AAP does not recommend these monitors. In fact, many parents who use them are less likely to put their babies to sleep safely and instead rely on the alarm to sound in the case of danger. This is not a good tactic, and monitors should not be used unless recommended by your pediatrician for particular health reasons (such as an oxygen requirement while sleeping).
Final Thoughts on Safe Sleep Guidelines for Babies
I hope these safe sleep guidelines and practices give you the info you need to have confidence as you create a safe sleep environment and set firm boundaries to protect your baby. Remember that you should always follow safe sleep guidelines and make sure that every caregiver does the same for every sleep.
Many risk factors are preventable, and you can significantly reduce your baby’s risk by following the safe sleep guidelines from the American Academy of Pediatrics. For the full list of guidelines, and to read the research in more detail, visit the recommendations from the American Academy of Pediatrics.
Ok, mama, let’s take a deep breath now. I know this is a stressful topic, but you have taken a big step in the right direction by reading up on these safe-sleep guidelines. I wish you and your baby sweet dreams and safe sleep! Read on for some frequently asked questions on this very important topic.
Frequently Asked Questions About Safe Sleep for Babies
You should always talk to your baby’s pediatrician about your baby’s sleep environment if you have any questions or concerns. And I’ve listed some commonly asked questions about these safe sleep guidelines below as well!
Are there warning signs for SIDS?
No, there are no warning signs or symptoms for SIDS. Follow safe-sleep guidelines to promote a safer sleep environment for your baby and to reduce their risks.
What if my baby falls asleep in the stroller or car seat?
The AAP does not recommend car seats, strollers, swings, infant carriers, and infant slings for routine sleep. Babies younger than 4 months are at higher risk because they may not be able to reposition themselves out of a potentially asphyxiating situation. If you’re out and about when your baby falls asleep in his car seat or stroller, just keep an eye on him until you can move him to a flat sleep surface. It’s common for babies to fall asleep in the car seat or stroller, so make sure they are not in a compromised position for breathing, and don’t allow them to sleep in there for too long or as a routine practice.
When can I stop worrying about SIDS?
SIDS/SUID typically peaks when babies are around 4 months old. Most cases occur before 6 months of age and then begin to taper. Technically, sudden unexpected infant deaths can occur at any time before the age of 1 year.
Are breathable crib mattresses safer than regular crib mattresses?
Breathable crib mattresses pass national safety standards and are safe to use for infant sleep. But the AAP also warns that there is no data to support the claim that they can reduce a baby’s risk of SIDS if your baby turns over in their sleep. Do not use a breathable crib mattress and place your baby on their stomach to sleep, for example.
If you are considering buying one, I’ve done a full analysis of breathable crib mattresses that I would encourage you to read before buying or using one, because I feel that there’s a lot of misleading information presented by the manufacturers of popular breathable crib mattresses.
Are co-sleepers and in-bed sleepers safe for sleep?
No. The AAP does not recommend in-bed sleepers such as the DockATot or other products because they have not been studied for safety. Bedside sleepers that meet CPSC safety standards may be an option, but there are no published studies that examine the products’ safety.
Are mesh bumpers safe for babies?
No. Crib bumpers are not safe, including the mesh kind. While they do allow air circulation, they are still an entrapment hazard. Avoid using any kind of crib bumpers.
Does mattress wrapping reduce SIDS risk?
There is a theory that came out of New Zealand, often referred to as the Richardson Hypothesis, which claims that toxic chemicals in crib mattresses play a role in sleep-related deaths. This theory has not received much support. In fact, the AAP discredits the theory, and a recreation of the study out of the UK disproves it.
But at the same time, there is some anecdotal support, so as a conscientious and probably over-worried mom, I cannot in my heart write it off completely.
So as long as you fully understand that this doesn’t currently have scientific backing, I want to list the recommendations here to simply allow you to make your own decision about your baby’s mattress and sleep environment.
So what is the Richardson Hypothesis? The theory states that accidental poisoning can occur when household fungus interacts with toxic gases from mattresses. These gases include phosphorus, arsenic, or antimony,which are chemicals that can be present in the mattress itself or in the flame retardant chemicals used in the mattress.
How would household fungus interact with these chemicals in a crib mattress? Fungus easily grows and accumulates when bodily fluids penetrate the mattress (such as diaper leaks or spit-up) or when temperatures rise (e.g., from body heat). The byproducts are the gases phosphine (PH3), arsine (AsH3), and stibine (SbH3).
A proponent of the theory, Dr. John Lee, MD, states:
These nearly odorless gases breathed even in small quantities for an extended time can interrupt the choline/acetylcholine transfer of nervous impulses from the brain to the heart and lungs. This shuts down the central nervous system; heart function and breathing stop. The gases are heavier than air, and about 1,000 times more poisonous than carbon monoxide.
But there isn’t research to support the claims, and again, this theory hasn’t been proven and doesn’t appear to hold weight. Still, as a prudent parent, in addition to improving the air circulation in your baby’s room, you can mitigate the “what ifs” in the back of your mind simply by using a non-vinyl waterproof mattress or polyethylene mattress cover. It’s easy enough to do so, and a waterproof mattress cover makes it easy to wipe up messes like diaper leaks and spit-up to prevent them from penetrating the mattress.
There are three different ways to do this, depending on the type of crib mattress you have:
Option A: Choose a safe waterproof crib mattress. Most mainstream waterproof mattresses have a PVC or vinyl waterproof barrier, but this is literally known as the most toxic plastic on the planet. If you want to buy a waterproof mattress, I recommend Naturepedic crib mattresses because they use food-grade polyethylene (rather than PVC/vinyl) for their waterproofing. Their crib mattresses are Greenguard Gold certified, but more importantly, they are GOTS certified, meaning they have the highest certification for organic crib mattresses.
Even if this theory holds no weight, by choosing a non-toxic waterproof mattress, you can safely avoid exposing your baby to a host of harsh chemicals, including phthalates, while they sleep.
Note: a lot of families buy secondhand baby products, but you should not buy a crib mattress secondhand because you won’t know the environment it was kept in, how old it is, and whether it contains mold or other contaminants. It’s likely safer to buy a new mattress, preferably for every child. If buying a new waterproof mattress isn’t an option for you financially, see option C below.
Option B: Use a non-toxic mattress cover on an organic crib mattress. If you have an organic crib mattress that isn’t waterproof, you do not need to replace it. (Just cross-reference my list of safe, organic crib mattresses to make sure it’s one of the safe brands I recommend.) If you have one of these mattresses that isn’t waterproof, you can simply use a protective mattress cover like the ones made by Naturepedic or My Green Mattress. I recommend having two of these on hand and rotate them out weekly or when they get soiled.
Option C: Use a polyethylene mattress wrap on a conventional mattress. If you have a conventional foam crib mattress and are unable to replace it with an organic one for financial reasons, you can use a non-toxic polyethylene mattress wrap to act as a barrier for any chemicals contained in the mattress, as well as bodily fluids that may penetrate the mattress (though most mainstream mattresses are now waterproof). However, please note that the AAP does not support this practice as a measure to protect against SIDS.
Thank you for reading this article on safe sleep guidelines for babies. If you found this helpful, please spread the word to other parents by sharing this article on your favorite social media platform!
Keep Reading:
- Toy Rotation: What It is, Why You Need One, and How to Get Started
- Let’s Get Real and Realistic About Screen Time Guidelines
- The Best Non-Toxic Bassinets and Co-Sleepers for Your Newborn
- The Best Non-Toxic Baby Furniture Brands
- What You Need to Know About Respectful Parenting









Leave a Reply